A life in pain: Soghra Walton’s story
“I have seen more physicians than I can count”
Soghra Walton spoke to GroundUp from her home near Rondevlei in Cape Town. Photos: Brenton Geach
In February, at a University of Cape Town Summer School talk about how to find help for persistent pain, a woman in the audience put up her hand during the Q&A session.
“I’m 73 and have reached the stage where my life is defined by pain. I wake up and I think to myself, ‘What am I going to do about it today? Do I take the pain pills? Do I try and see someone?’ I anticipate it. I fear it. I put things off because of it,” she said, and confessed that she had come to deeply mistrust the medical community.
“The last person I saw was a neurologist, who basically said, ‘You don’t tell me what to think. I am the neurologist.’ I have seen more physicians than I can count. I have visited three private pain clinics, but without finding any sustained relief.”
The panel of experts seated at the foot of the lecture theatre included an anaesthetist, a GP, a physiotherapist, a psychologist and a psychiatrist. They were quick to sympathise.
“That’s awful, and we recognise that,” said the chairperson.
“I think the key question that you’re asking is, how do you begin to deal with such persistent suffering, when so many attempts have already failed? Who do you start with?”
She ventured that it might help to try to identify the biggest impacts of pain.
“What upsets you the most about how pain interferes in your life? What bits of your life are you wanting to restore? That will often help you to identify who to work with first.”
Examples were given. A person wanting to re-engage with the meaningful things in their life might do well to speak to an occupational therapist who understands pain. Someone whose pain has caused them to become ratty and anxious could consider working with a mental health professional, and so on. All agreed that the specialist should ideally be working in a team with other health professionals.
“And that team should make you feel that you are involved in the planning, and are part of the decision-making,” said the chairperson, before moving on to the next question.
The woman nodded, folded her hands.
I introduced myself afterwards and explained that I was writing a series of articles about pain. The woman, introducing herself as Soghra, wrote down her number, and invited me to visit her at home, in Zeekoevlei.
Weeks later I pull up outside a spacious home alongside the Rondevlei reserve.
Soghra Walton ushers me in.
“Before I say anything, I want you to know that I haven’t always thought of myself as a person who is always in pain. For much of my life I did things - I worked, I was a busy girl. But in recent years this history of mine has gotten the better of me,” she says, drawing on a cigarette at her dining room table. In the background an African Grey parrot occasionally whistled a tune.
“The body keeps the score,” I say awkwardly, repeating the title of Dr. Bessel van der Kolk’s bestselling book The Body Keeps the Score: Brain, Mind, and Body in the Healing of Trauma, in which he examines how traumatic stress literally rearranges the brain and body, storing memories as physical sensations rather than narratives, and highlighting that trauma causes lasting emotional, physical, and cognitive damage, requiring healing methods that address the body.
Soghra says she’ll start at the beginning. She was born in 1953, in Cape Town, the only girl among four siblings. It was a stern but not unhappy childhood.
At the University of Cape Town and later the University of the Western Cape Soghra trained as a psychiatric social worker. Her experience of working at Groote Schuur in the 1960s, and later at the William Slater Centre in Rondebosch, was bruising.
“The white patients wanted nothing to do with a black person, and the white bosses did not view me as a social worker but rather as a potential plaything, or nanny for their children,” she says.
Soghra hung out with anti-apartheid activists, and later eloped to Botswana with a white Afrikaner: “One of those Bob Dylan types with a guitar and a drug problem, which was very attractive at the time. I thought: ‘Here is a person who understands me, or perhaps can just take me away.’”
Their relationship was characterised by “horrible abuse, culminating in part of my skull being fractured after he slammed my head into a wall”.
Realising that she would need to raise their two young children on her own, Soghra talked her way into a job as a construction buyer, which she found she had a talent for.
Then she fell ill.
“I urgently returned to Cape Town and my mother checked me in to Tygerberg Hospital, where I was diagnosed with cervical cancer, and was told I needed a hysterectomy. I went into menopause two days later, at the age of 27 years,” says Soghra. She was not offered hormone replacement therapy (HRT), today a standard recommendation for women who go through early menopause. As a consequence, her bones became brittle and broke easily, and she was diagnosed with type 2 diabetes.
The realisation that her health had been compromised by less than ideal care only dawned much later in life. In the intervening years she met and fell in love with Roger Walton, an English engineer employed in Botswana’s mining industry, who became a doting father to the children. They maintained active lives, hiking every chance they got, including in the Kashmir Valley. They returned to Cape Town and opened a successful electrical company.
Soghra continues to search for relief from pain. Photo: Brenton Geach
Soghra was happy, but at the age of 40 she found she was taking a lot of medication: oestrogen tablets, diabetes medication, and more. She would see the trusted family physician, but there were cultural limits to the care he could provide, “things an Indian woman should simply not bring up with a male Indian doctor”.
“As a person, as a medical subject, I come with context, but no single person understood this context. I probably didn’t understand it myself,” she says.
Sograh decided to go back and study, and in 2003 submitted her Master in Philosophy thesis to the University of Western Cape: An Exploration of the Socio-Cultural Influences of Traditions on the Assimilation of Indian Women into the Western Cape Society.
Friends encouraged her to write about her life and she says she started to feel “lighter”. Physically, however, she was collapsing, specifically her cervical vertebrae, which had to be reconstructed using a titanium cage.
“When they put it in they damaged the C7 nerve, which no neurosurgeon wanted to operate on because of the high risk of permanent damage,” says Soghra, taking a drag on her cigarette.
“I realized I was badly damaged, both physically and psychologically. I had paid tens of thousands to neurosurgeons. I saw several psychologists, who all dismissed me. I found no relief.”
In 2014, she suffered a heart attack, and had a stent put in an artery. She was prescribed Capotril, a medication that improves survival chances after a heart attack by relaxing blood vessels to improve blood flow.
“I recovered but I was left with huge headaches from the medication. My neurologist called the cardiologist to ask what he would suggest, and the cardio said, ‘You’re the brain doctor, you decide,’ a prime example of how everyone in the private health system operates in their own little silos.”
By this time, the cost of Soghra’s care was becoming astronomical.
“The moment you want to involve more people in your care, especially if it means seeing mental health practitioners, your medical aid tells you, ‘Sorry, major depression is not a prescribed minimum benefit.’ You get two visits to a psychologist, and that’s the end of your depression management, unless you pay for it out of your savings scheme,” she says.
Some years before, Soghra and her husband had started a shelter for women in their community, “a project very close to my heart, which I had to step back from while I recovered.”
When she was back on her feet, she found her staff had looted the finances.
“I was devastated. We closed it down. I fell into depression. I have been a lifelong believer in social action, in doing things for the community that nobody else is doing, but now I resigned myself to a life of just managing my pain. I had a back that didn’t work, numbness in many places due to nerve damage. Layer on layer on layer.”
At times, Soghra says she self-medicated.
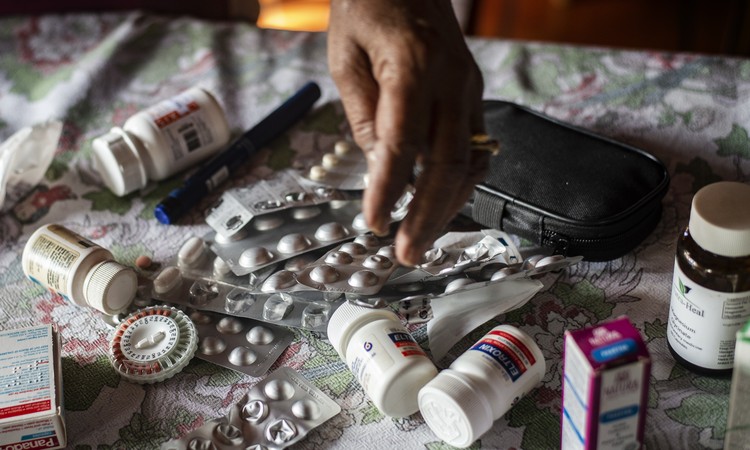
“I have an apothecary in my room that skrik for niks,” she says.
“I have never been a fearful person, but in recent years I have at times been paralysed with fear, to the extent that I couldn’t get out of bed,” says Soghra, who admits to becoming tetchy and reactive with those around her.
Soghra had another heart attack last year – “a massive one” – and the fact that she had reported to a major private hospital in the area before it happened, only to be discharged with a diagnosis of bronchitis, fuelled her growing distrust of medical professionals.
“I reached a point where I questioned everything that anyone said. I was full of self-doubt, too, wondering is this all in your head? Is it psychosomatic? I came to see that actually I was a traumatised person, and my husband was also a traumatised person,” she says, adding that doctors, if she arrived on her own for an appointment, would often ask why her husband wasn’t present.
“I have an apothecary in my room that skrik for niks,” says Soghra. Photo: Brenton Geach
“In Afrikaans there’s this lovely word – geldigheid – meaning validity. This went to the heart of my validity as a person. It was like they expected him to bring me in, like taking a dog to the vet,” she says.
Soghra and Roger decided to drop everything and take a trip up the west coast, into Namibia.
“I was in pain the whole time, in my back and hip.”
On their return, Soghra consulted yet another neurosurgeon. She had started carrying a timeline of her medical issues into every consultation, which she now pushed across the table.
“He looked at my story, and said, ‘Nobody is going to touch you, there’s too much history’ There is nothing I can do for you.’”
Driving home, she says she closed her eyes and prayed.
“I said to the gods, or to God, ‘I am out of ideas, I am going to leave this with you now’, and just then an advertisement came on the radio for a talk at the University of Cape Town Summer School, about how to get help for pain. And I thought to myself, I am going to go along, and see if there’s someone there that I can talk to. And that’s where I met you.”
Sograh hasn’t yet found a medical professional she trusts, “someone who is willing to look at the whole picture”.
Her search for solutions continues.
Support independent journalism
Donate using Payfast

Don't miss out on the latest news
We respect your privacy, and promise we won't spam you.
Next: South Africa’s giant pain problem
Previous: US funding cuts put Cape Town users at risk of not getting vital medicine
© 2026 GroundUp. This article is published under the GroundUp Republication Licence Version 1.0. Email info@groundup.org.za to request permission to republish.