US funding cuts put Cape Town users at risk of not getting vital medicine
Streetscapes stepped in to help foot the bill for methadone costs after access issues at some centres
After spending his 40th birthday on the streets in 2022, Jade Lewis says he decided to get help for his heroin addiction. He is one of many people who use methadone distributed by organisations such as the TB HIV Care. Photos: Marecia Damons
- People using methadone to recover from their dependencies on opioids like heroin and prescription painkillers have raised concerns about the inconsistent access to this lifesaving medication.
- One person, who regularly collects methadone weekly from TB HIV Care’s drop-off centre in Cape Town, says he has been turned away several times without any medication or only enough for a couple of days.
- TB HIV Care, a non-governmental organisation, says there is no indication of national shortage of methadone. It says delays were due to a “transition in funding”.
- US funding cuts to health care across the world last year have left many organisations providing essential services, like TB HIV Care, scrambling and competing for dwindling amounts of money.
When Jade Lewis went to collect his methadone at a TB HIV Care drop-off in Cape Town, he expected to leave with the medication helping him rebuild his life. Instead, he was told to come back another day.
Lewis, 44, has been battling heroin addiction since 2005. He explained that this delay in accessing methadone put his recovery at risk.
Methadone is used to help people recovering from opioid dependency, including heroin and prescription painkillers. It is effective and life-saving.
In February, Lewis went to make his weekly collection at the TB HIV Care drop-off on Adderley Street but was told no methadone was available. This happened again in April. He takes 7ml per day.
Over the weeks that followed, supply was inconsistent, he said. Sometimes he received enough for three days, sometimes for two. During gaps, he says he used heroin to manage withdrawal symptoms.
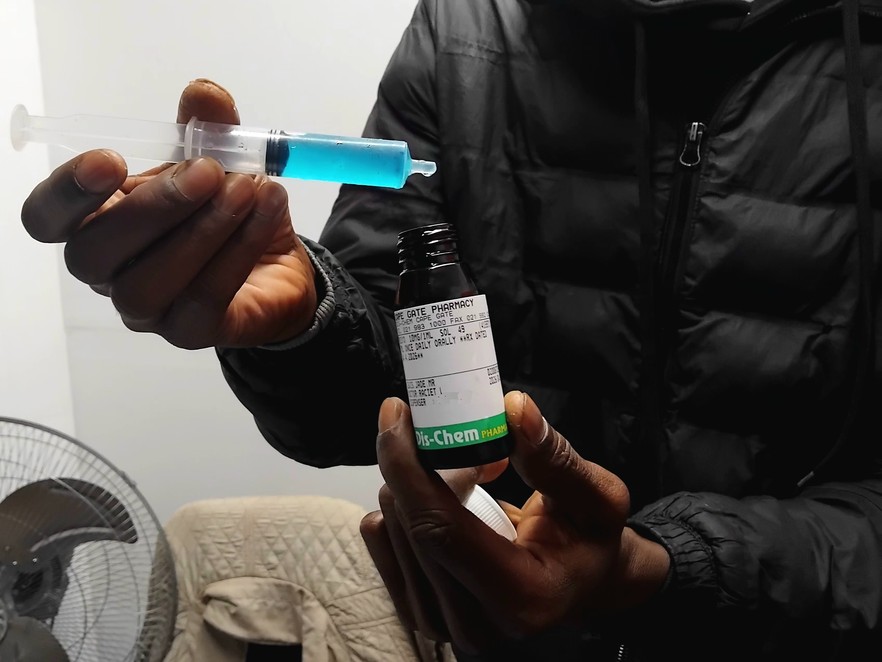
Earlier this month, Lewis and Streetscapes peer outreach facilitator Rudie Basson went to a private doctor for a prescription. Streetscapes helped cover the cost of the methadone from a pharmacy, about R283 to last five days.
Lewis, who grew up in Mitchells Plain, has had a decades-long battle with substance use. He first used cocaine in 2001. “When I couldn’t afford cocaine anymore, I started using tik and then heroin in 2005. In that year my whole life changed … I still had a good job. I worked for the government and managed to maintain my job. But it slowly started consuming me.”
Lewis takes 7ml of methadone daily. When he was unable to access the medication at TB HIV Care, Streetscapes covered the costs of purchasing methadone for him from Dischem.
An incident of sexual assault in matric, grief over his sister’s death in 2011, and the collapse of his marriage in 2019 exacerbated his dependence on heroin, he said.
Lewis said he has been in and out of recovery programmes since 2014.
In November last year, he again enrolled in the methadone programme through TB HIV Care and Streetscapes.
He currently stays at a shelter for adults and earns a stipend from work at Streetscapes and by wrapping bags for long-distance bus travellers.
Lewis said the methadone disruptions also cost him a job opportunity because he needed a month’s supply of methadone but was told there was no methadone available to give him. “I had to let the opportunity go,” he said. “That incident threw me off, and I started to use heroin again.”
Describing his withdrawals without methadone, he said: “Your body shakes, you get spasms. You feel hot and cold. You don’t know up from down. You can’t concentrate or focus. It starts with light shocks in your head and moves through your body.”
When GroundUp visited TB HIV Care’s drop off centre on 22 April, this sign was on the wall at the entrance.
Basson, who works with Streetscapes’ clients, said any disruptions in methadone access leave people with few options. “They might not have the money to buy methadone because it’s expensive. For 35ml it costs about R200 to R300. Heroin is cheaper to buy,” he said.
US funding cuts
TB HIV Care’s People Who Inject Drugs programme was previously funded by the US Presidents fund (know as PEPFAR) via the US Centres for Disease Control and the Global Fund to Fight AIDS, TB and Malaria (a fund that is contributed to by countries and private donors across the world).
Since US funding for global health has been slashed by the Trump administration there has been much more competition for resources. For example, the Global Fund’s current allocation to South Africa is only a quarter of its previous three-year cycle.
TB HIV Care has had to compete for much dwindled funding, making it hard to sustain essential services like the methadone programme.
But the good news is that TB HIV Care appears to now have access to funds to keep the programme going.
TB HIV Care communications manager Aziel Gangerdine said the organisation “is aware of recent concerns regarding the availability of methadone”.
“At this stage, no official announcement from South African regulatory authorities indicating a national shortage of methadone was announced.”
He said recent funding changes had required adjustments. “The People Who Use and Inject Drugs Programme, implemented by TB HIV Care with support from international donors, recently underwent a transition in funding. As a result, certain operational and process adjustments were required, which temporarily affected service momentum in some areas”.
“These operational matters have since been addressed, and service delivery has stabilised,” Gangerdine added.
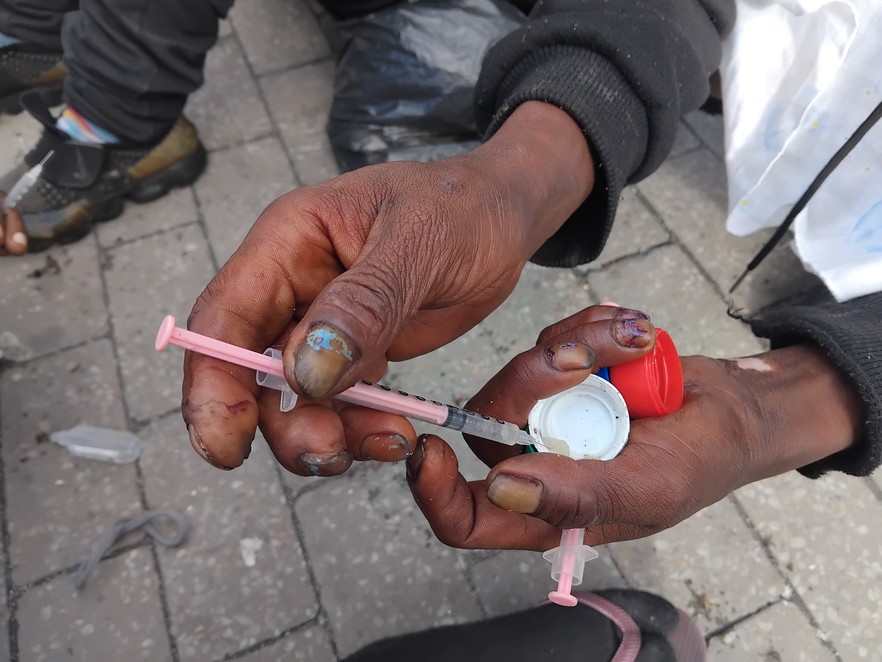
A heroin user prepares a dose for injection.
Support independent journalism
Donate using Payfast

Don't miss out on the latest news
We respect your privacy, and promise we won't spam you.
Next: A life in pain: Soghra Walton’s story
Previous: Cape Town struggles to relocate Khayelitsha families living on sinkholes
© 2026 GroundUp. This article is published under the GroundUp Republication Licence Version 1.0. Email info@groundup.org.za to request permission to republish.